It’s considered best practice to assess benefits and risks before taking part in any medical procedure. After discovering DXA technology, clients commonly become curious about any risks involved. “Am I being exposed to a harmful level of radiation during a DEXA scan?” It’s a smart and valid question, and the short answer is: not much, if any. Let’s break down the science behind medical imaging to learn the full story of DXA technology.
Medical Imaging Technology
More than 120 years ago, scientists discovered early elements of what became precursors to medical imaging technology used today. In 1895, the first X-ray was developed by Wilhelm Roentgen in Germany after observing rays from a cathode ray tube could penetrate human flesh (but not bones). X-ray technology began to advance over the early part of the 20th century and soon became the widespread standard for bone imaging.
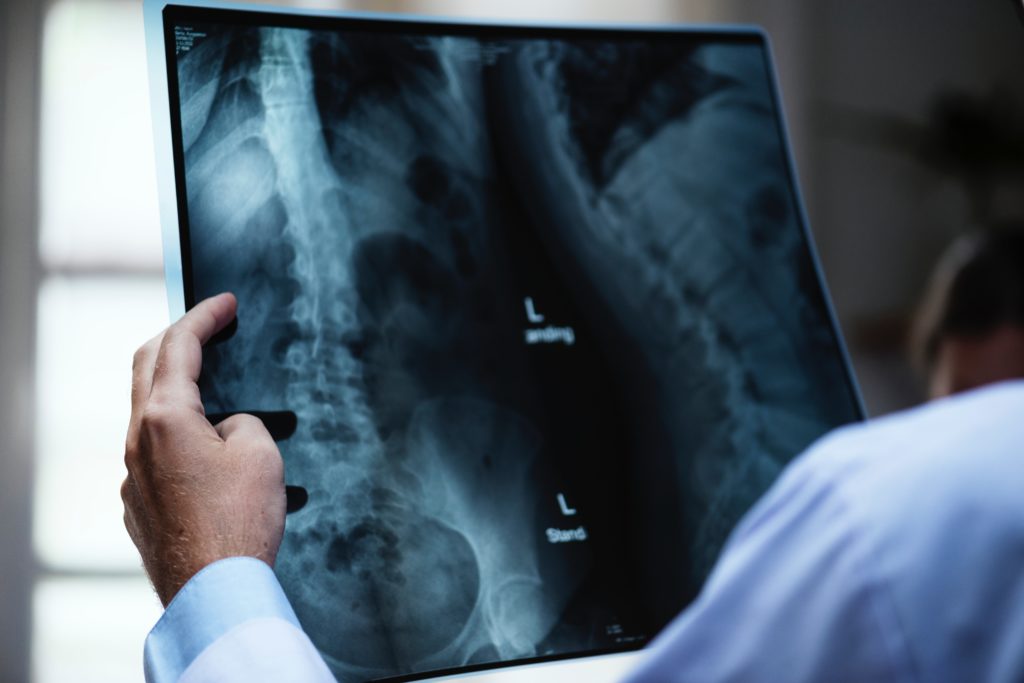
As X-ray imaging – and computer availability – progressed throughout the 1960s, computed tomography (CT) entered as a more practical application of X-ray technology. CT scanning uses computer-processed combinations of X-ray measurements from different angles (slices) to produce a comprehensive image of structures inside the body. In addition to CT scanning, medical professionals have access to even more advanced imaging techniques including PET, MRI and MRS technology that can observe the body at the cellular level.
DXA (Dual-energy X-ray absorption) emerged onto the medical imaging scene much later in the 20th century, being first introduced in 1987. DXA scanning takes two X-ray beams with different energies and projects them onto a patient’s body, often while the individual lies on a flat-bed device as an arm passes over their body from head to toe, providing a full picture of body composition. Soft tissue absorption is subtracted from full-body tissue absorption to estimate a measurement of bone mineral content (density). The technology is primarily used to assess bone health and risk for osteoporosis, but it also gives incredibly accurate picture of lean mass and body fat.

Assessing Risk
Scientists did not begin to consider the possibility of harmful exposure from X-rays until many years after it was implemented in medical practice. Today we have a better sense of risk from radiation exposure which is considered during examination and treatment of patients who require significant amounts of imaging. Although X-rays can cause DNA mutations that have been cited to lead to cancers later in life, researchers agree the benefits vastly outweigh the risks.
Cosmic radiation naturally occurs in the atmosphere (but is mostly blocked in space before reaching the Earth) along with other forms of radiation from the breakdown of uranium in rock, soil and water. Research suggests the average effective dose from natural background radiation is 2.4 mSv/year worldwide. (mSv, or millisievert, is the scientific unit often used to measure effective dose of radiation, which is calculated using the absorbed dose to tissues exposed to X-rays and the relative radiation risk assigned to the tissue.)

The DXA Difference
So how do X-ray, CT and DXA exposure compare? While actual radiation exposure depends on the device, duration of a scan, location of scan, and the subject’s size, literature suggests a single chest CT scan delivers 70 times as much exposure as a chest X-ray (0.1 mSv versus 7 mSv). A full-body CT scan delivers around 12 mSv, while a DXA scan delivers just .0046 mSv on average. DXA technology, therefore, emits a significantly less effective radiation dose, if any at all when compared to other imaging devices.
It’s always smart to consider risk in any procedure alongside the benefits. Data collected from DXA scanning technology provides an accurate, detailed look into bone density as well as lean mass and subcutaneous and visceral fat. These factors can paint a more comprehensive picture of health than can be determined from other body composition devices. This information can pave the way towards a healthier lifestyle and possibly prevent diseases associated with high body fat if appropriate interventions are implemented.
Find out more about DEXA scanning and schedule a visit with one of our experts near you.



